Procedure of PSMA Therapy at Theranosticum Vienna
PSMA therapy is a structured treatment process that is performed on an outpatient basis at our center. Many patients want to know in advance what to expect—how long the appointment takes, which steps are involved, and what needs to be considered after the infusion.
The therapy itself is technically well defined and follows standardized medical procedures. Each treatment is preceded by a careful evaluation of the indication for PSMA therapy. Only when the medical prerequisites are fulfilled is the treatment planned.
A single treatment session usually lasts 2 - 3 hours and includes a medical consultation, the infusion of the radiolabeled therapeutic agent, and a short observation period. The procedure is carried out on an outpatient basis—inpatient admission is typically not required.
In this article, you will find a transparent overview of all steps before, during, and after the therapy.

Before Therapy – Preparation and Medical Consultation
Before the first cycle of PSMA therapy, a detailed medical consultation takes place. This serves to clarify any open questions, explain the procedure in an understandable way, and ensure that all medical prerequisites are fulfilled.
During this appointment, we discuss with you:
- The previous course of the disease
- Current findings, particularly PSMA PET/CT
- Relevant laboratory values
- Possible comorbidities or special considerations
You will also receive important informational documents, including:
- Patient information about the therapy
- An informed consent form
- An information sheet with radiation protection guidelines
- Organizational details for the treatment day
Our consultation provides space for your individual questions. The goal is to ensure that you understand the procedure and feel well prepared for the day of treatment.
The specific therapy appointment is scheduled only once all prerequisites are met and any open questions have been clarified.

On the Day of Therapy
PSMA therapy is performed on an outpatient basis at Theranosticum Vienna. The entire stay typically lasts about two to three hours.
Placement of an Intravenous Access
At the beginning, a venous access (e.g., via a vein in the arm) is established. This access is used for both preparatory infusions and the administration of the therapy itself.
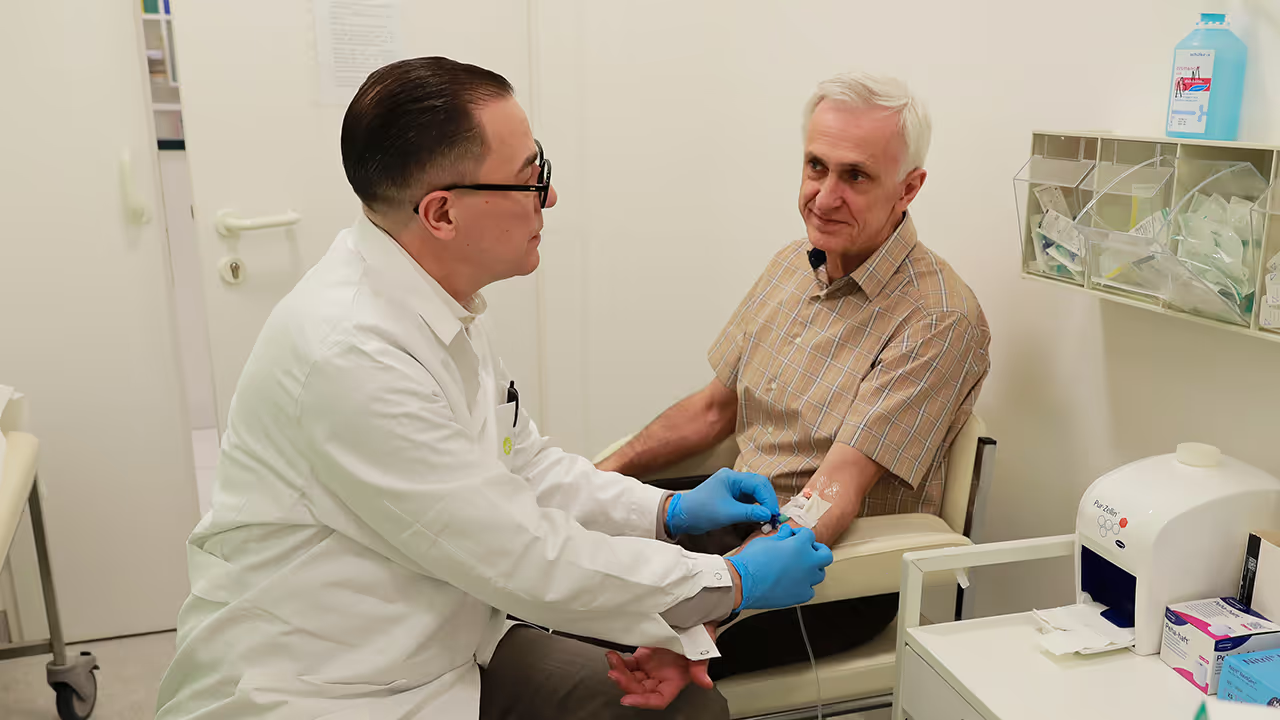
Preparatory Infusions
Before administration of the radiolabeled therapeutic agent, you will receive prophylactically:
- A medication against nausea (e.g., ondansetron)
- A gastric protection agent (e.g., pantoprazole)
These measures help to further improve the tolerability of the treatment.
Infusion of Lutetium-177 PSMA
The therapeutic agent—most commonly Lutetium-177 PSMA—is then administered intravenously. The infusion itself takes approximately 15 to 20 minutes.
You will be medically supervised throughout the entire process. The treatment is carried out under controlled conditions and according to standardized nuclear medicine protocols.
After completion of the infusion, the post-treatment observation phase begins.
After Therapy – Monitoring and Discharge
After completion of the infusion, you will remain in the treatment area for a short period of observation. During this phase, it is assessed whether you have tolerated the therapy well and whether any immediate symptoms occur.
This is followed by a final medical consultation. During this discussion, the next steps are outlined, in particular:
- Recommended behavioral precautions
- Follow-up examinations
- The planned date for the next treatment cycle
Before discharge, a so-called release measurement is performed. This involves checking, at a defined distance, the level of residual radiation emitted by the body. Outpatient discharge is only permitted once the legally required threshold values are met.
You will also receive:
- An information card to carry with you in daily life
- A brief medical report for further care
- Organizational information for the coming days
In most cases, inpatient admission is not required. Once all checks have been completed, you can leave our center.

Radiation Protection After PSMA Therapy – What Should You Keep in Mind?
After PSMA therapy, a small amount of residual radioactivity from Lutetium remains in the body for a limited period. This decreases continuously and is additionally excreted via the urine.
To minimize radiation exposure to others, certain precautions should be followed during the first days after treatment. These will be explained to you in detail during the consultation.
Key recommendations for the first approximately 10 days:
- Reduce close and prolonged physical contact, especially with pregnant women and young children
- Avoid extended periods in close proximity to others (e.g., at events)
- Use the toilet while seated and ensure thorough flushing
- Wash your hands carefully after using the toilet
- Drink sufficient fluids (at least about 1.5 liters per day) to support excretion
Short everyday contact is generally not a concern. These measures are primarily precautionary and are limited to a defined period of time.
You will also receive an information card to carry with you for a certain period. If you require medical treatment or visit a hospital during this time, inform the medical staff about your recent therapy.
Treatment Cycles – How Often Is PSMA Therapy Performed?
PSMA therapy is administered in multiple treatment cycles. The goal is to achieve a sufficient therapeutic effect while carefully monitoring tolerability.
In most cases, three treatment cycles are initially planned. These are typically carried out at intervals of about four to six weeks. This time interval allows the body to recover between treatments and provides the opportunity to monitor laboratory values and the clinical course.
After the third cycle, a repeat PSMA PET/CT scan is usually performed. This so-called interim assessment serves to objectively evaluate the response of the disease.
Depending on the findings, tolerability, and overall course, additional treatment cycles may follow. In many cases, up to six cycles are performed in total. However, the exact number depends on the individual situation.
There is currently no universally defined fixed maximum cumulative dose. Continuation of therapy is always based on a structured medical evaluation.
Monitoring Between Treatment Cycles
Between the individual cycles of PSMA therapy, regular medical check-ups are carried out at our institute. These serve to assess the response of the disease and to detect any changes at an early stage.
Typically, the following parameters are monitored:
- PSA level as a tumor marker
- Blood counts (red and white blood cells, platelets)
- Kidney function values
- Additional laboratory parameters, if required

These follow-up assessments are carried out in close coordination with the treating urologist or oncologist. In certain situations, additional imaging—such as PSMA PET/CT—may be required.
Regular monitoring allows the therapy to be continued responsibly, adjusted, or, if necessary, discontinued. The goal is to continuously maintain a balance between therapeutic benefit and tolerability.

What Should I Consider Before PSMA Therapy?
Before starting PSMA therapy, several medical and organizational aspects are evaluated. The goal is to ensure that the treatment can be carried out safely and that potential risks are identified at an early stage.
Please inform our treating team in particular if:
- There is a known impairment of kidney function
- Significant abnormalities in blood counts are present
- Chemotherapy or radiation therapy has recently been performed (within the last few weeks)
- Urinary incontinence, a catheter, or a stoma is present
- Severe dry mouth is present
- Acute infections or serious comorbidities exist
Some of these factors may influence the planning or execution of the therapy. They do not automatically mean that treatment is not possible, but they must be taken into account in the decision-making process.
It is also important to be willing to follow the recommended radiation protection measures after therapy. This includes, in particular, temporarily reducing close contact with others and carrying the information card after discharge.
Frequently Asked Questions About the Procedure of PSMA Therapy
Is PSMA therapy performed on an inpatient or outpatient basis?
PSMA therapy is usually performed on an outpatient basis. Inpatient admission is generally not required, but may be possible in individual cases. After the infusion and a short observation period, patients can leave our facility.
How long does a PSMA therapy appointment take?
An appointment typically lasts about two to three hours. It includes the medical consultation, preparatory infusions, administration of Lutetium-177 PSMA, as well as post-treatment observation and release measurement prior to discharge.
Is the infusion painful?
The therapy is administered via a venous access in the arm. The infusion itself is generally not painful. Most patients find the procedure well tolerated.
Can I drive after the therapy?
In most cases, driving is possible as long as you feel well and no symptoms occur. Individual recommendations will be provided during the medical consultation.
Do I need to isolate myself after the therapy?
Full isolation is not required. However, for approximately ten days, certain radiation protection measures should be followed—especially with regard to pregnant women and young children.
When does the next treatment cycle begin?
The next cycle is usually scheduled at an interval of four to six weeks. Prior to this, laboratory tests and, if necessary, imaging—such as PSMA PET/CT - are performed.
Who performs the monitoring between cycles?
Monitoring can be carried out in close coordination with the treating urologist or oncologist. Parameters such as PSA levels, blood counts, and kidney function are assessed.
We take time for what matters - your care
If you have questions or would like to schedule an appointment, we are here for you.
In a personal consultation, we discuss your concerns in a calm setting and outline the next steps together.
Our team will get back to you promptly and support you competently and reliably - from the first contact through to your therapy appointment.




