PSMA PET/CT – Precise Diagnostics for Prostate Cancer

What Is PSMA PET/CT Imaging?
PSMA PET/CT is a specialized nuclear medicine imaging technique that allows prostate cancer cells to be visualized with high precision. It is based on the so-called prostate-specific membrane antigen (PSMA)- a protein that is present in increased concentrations on many prostate cancer cells.
For the examination, a radiolabeled PSMA ligand is administered via a vein. This substance binds specifically to tumor cells. The PET technology then makes it possible to visualize where these cells are located within the body. In combination with CT, a highly detailed whole-body image is created, showing both biological activity and anatomical structures.
For you, this means that even very small lymph node or bone metastases can be detected—sometimes even before they become visible on conventional imaging (for example, bone marrow metastases).
PSMA PET/CT is used for precise staging and for evaluating a renewed rise in PSA levels. It often provides the key information needed to guide further treatment planning.
When Is PSMA PET/CT Imaging Useful?
At Initial Diagnosis with Increased Risk
If certain risk factors are present at the time of initial diagnosis—such as a high PSA level or an unfavorable Gleason score/ISUP grade—PSMA PET/CT can help to more accurately determine the true extent of the disease.
For you, this means: It can be identified at an early stage whether the tumor is confined to the prostate or whether lymph nodes or bones are already affected. This information plays a key role in determining the most appropriate treatment strategy.
In Case of a Rising PSA Level (Biochemical Recurrence)
A renewed rise in PSA after surgery or radiation therapy can understandably be a source of concern. In this setting, PSMA PET/CT offers particularly high sensitivity - even at low PSA levels.
The prospective proPSMA study (Hofman et al., The Lancet, 2020) demonstrated that PSMA PET/CT is significantly more accurate than conventional imaging in high-risk patients (92% vs. 65% diagnostic accuracy).
For you, this means: A potential recurrence can often be detected earlier and localized more precisely—providing the basis for targeted treatment.
Before Planned PSMA Radioligand Therapy
Before PSMA radioligand therapy is considered, it must be confirmed that the tumor cells sufficiently express PSMA. PSMA PET/CT is therefore used not only for diagnosis, but also as an important decision-making tool in treatment planning.
Whether PSMA PET/CT is appropriate in your individual situation depends on your PSA dynamics, previous treatments, and the specific clinical question. A structured evaluation of your findings by our expert team helps to clearly define the next steps together in a transparent and understandable way.
How Reliable Is PSMA PET/CT?
PSMA PET/CT is one of the most extensively studied imaging modalities in modern prostate cancer diagnostics. Its high diagnostic accuracy is well established by numerous prospective studies and meta-analyses.
A key study is the randomized, multicenter proPSMA trial (Hofman et al., The Lancet, 2020). In patients with high-risk prostate cancer, PSMA PET/CT demonstrated significantly higher overall accuracy compared to conventional imaging (CT and bone scintigraphy). Diagnostic accuracy reached 92%, compared to 65% with standard imaging methods. In addition, PSMA PET/CT more frequently led to changes in the planned treatment strategy.
In the setting of biochemical recurrence—meaning a renewed rise in PSA following surgery or radiation therapy—systematic reviews also show high detection rates. A meta-analysis published in European Urology describes increasing detection rates with rising PSA levels, while still identifying clinically relevant findings even at low PSA concentrations.
These data explain why PSMA PET/CT is increasingly recommended in international guidelines for specific indications - particularly for precise staging and for the evaluation of suspected recurrence.
Advantages of PSMA PET/CT Compared to CT, MRI, and Bone Scintigraphy
In the evaluation of prostate cancer, imaging methods such as CT, MRI, or bone scintigraphy are commonly used. These techniques primarily visualize anatomical changes—such as enlarged lymph nodes or visible alterations in bone structure.
PSMA PET/CT goes a step further: it not only visualizes anatomical structures but also detects active tumor cells at the molecular level. Tumor lesions are identified based on their PSMA expression - regardless of whether they are already visibly enlarged.
For you, this means: Even small metastases can be detected before they become apparent on conventional imaging. This can be crucial when it comes to choosing the right treatment at the right time.
Key Advantages of PSMA PET/CT at a Glance:
- Higher diagnostic accuracy compared to conventional imaging
- Earlier detection of lymph node and bone metastases
- Whole-body imaging in a single examination
- A more precise basis for individualized treatment planning
In cases of rising PSA levels or at the time of a high-risk initial diagnosis, this increased sensitivity can help reduce uncertainty and support more targeted treatment decisions.
If PSMA PET/CT reveals more advanced disease, this may have immediate implications for treatment planning—for example, regarding systemic therapy or the potential use of PSMA radioligand therapy.
What to Expect During a PSMA PET/CT Scan
The procedure for a PSMA PET/CT scan typically follows these steps:
Preparation
In most cases, no special fasting is required. You may eat and drink as usual, unless you receive specific instructions otherwise. Your regular medications can generally be continued. Before the examination, you will receive all relevant information.
Injection of the PSMA Tracer
At the beginning of the examination, a radiolabeled PSMA ligand (for example, Gallium-68 or Fluorine-18) is administered via a vein. This substance circulates throughout the body and binds specifically to PSMA-expressing tumor cells.
This is followed by a waiting period of approximately 45 to 60 minutes, allowing the tracer to distribute optimally in the body and accumulate in tumor tissue.
Imaging
The actual PSMA PET/CT scan typically takes about 10 to 20 minutes. During this time, you will lie still on the examination table. The scanner acquires a whole-body image that visualizes both molecular activity and anatomical structures.
The examination itself is not painful—apart from the brief needle insertion for the injection.
After the Examination
After the scan, you can usually leave the facility shortly thereafter. The tracer decays within a few hours and is primarily excreted via the kidneys. No clinically relevant long-term radioactivity remains in the body.
For most patients, PSMA PET/CT is less burdensome than they initially expect.
Radiation Exposure and Safety of PSMA PET/CT
Concerns about radiation exposure are understandable—especially if multiple imaging studies have already been performed. For this reason, PSMA PET/CT uses a carefully calculated, medically standardized dose of a radiolabeled tracer.
The level of radiation exposure - depending on the tracer used and the CT protocol - is comparable to that of other diagnostic CT examinations.
What is essential is that the examination is only recommended when the expected medical benefit clearly outweighs the potential risks. In cases of suspected metastasis or biochemical recurrence, the additional diagnostic accuracy can be crucial for treatment planning.
What You Should Know:
- The administered activity is individually calculated
- Allergic reactions to PSMA tracers are not known to date
- The tracer decays within a few hours
- It is primarily excreted via the kidneys
- No clinically relevant long-term radioactivity remains in the body
Overall, PSMA PET/CT is considered a well-tolerated and safe procedure. Before the examination, you will receive a medical consultation in which any individual risks are discussed.
Overall, PSMA PET/CT is considered a well-tolerated and safe procedure. Before the examination, you will receive a medical consultation in which any individual risks are discussed.
What Do the Results of a PSMA PET/CT Mean?
After the examination, the key question arises: What do these findings mean for me personally?
PSMA PET/CT shows whether and where active prostate cancer cells are present in the body. This information plays a central role in guiding further treatment planning.
No Evidence of Metastases
If no PSMA-positive lymph nodes or distant metastases are detected, this suggests that the disease is confined to the prostate. In this situation, curative treatment options such as surgery or radiation therapy are often the primary focus.
Detection of Lymph Node Metastases
If affected lymph nodes are identified, this may influence the treatment strategy. Depending on the extent of disease, targeted radiation therapy, extended surgery, or systemic treatment may be appropriate.
Detection of Bone or Organ Metastases
If metastases are present in the skeleton or other organs, the disease is considered systemic. In this case, systemic therapies become the main focus—such as hormone therapy, chemotherapy, or, where appropriate, PSMA radioligand therapy.
Why Interpretation Is Crucial
PSMA PET/CT does not provide an isolated snapshot but is part of a comprehensive clinical assessment. PSA dynamics, Gleason score/ISUP grade, and prior treatments must all be taken into account. The goal is to avoid overtreatment while ensuring that necessary steps are taken without delay.
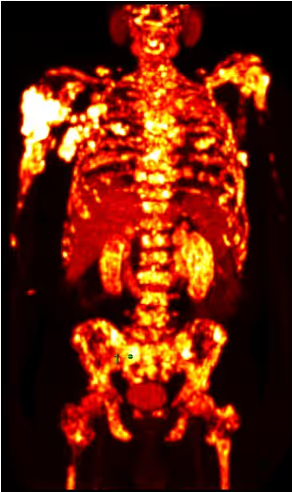
PSMA PET/CT at Theranosticum Vienna
PSMA PET/CT delivers its full value only when the results are precisely interpreted and placed in the context of the individual disease course. What matters is not only the imaging itself, but the medical assessment within the overall clinical picture.
At Theranosticum Vienna, PSMA PET/CT imaging is performed using advanced hybrid technology and standardized examination protocols. Particular emphasis is placed on:
- High-resolution whole-body imaging
- Structured, guideline-based reporting
- Integration of PSA dynamics, histology, and prior treatments
- Interdisciplinary evaluation of complex cases
A key advantage lies in the close integration of diagnostics and therapy. If PSMA PET/CT indicates advanced or metastatic disease, it can be immediately assessed whether further treatment - such as PSMA radioligand therapy - is medically appropriate.
Our goal is to provide a clear and well-founded recommendation for the next steps—evidence-based and tailored to your individual situation.
Frequently Asked Questions About PSMA PET/CT (FAQ)
How Long Does a PSMA PET/CT Scan Take?
You should plan approximately 1.5 to 2 hours for the entire PSMA PET/CT examination. After the tracer injection, there is a waiting period of about 45–60 minutes. The actual imaging itself takes around 20 minutes.
Is a PSMA PET/CT Scan Painful?
No. The examination itself is not painful. Only the intravenous injection of the tracer involves a brief needle insertion - similar to a routine blood draw.
At What PSA Level Is PSMA PET/CT Useful?
PSMA PET/CT can be particularly useful in the setting of biochemical recurrence—that is, when PSA levels rise again after surgery or radiation therapy. Studies show that clinically relevant findings can be detected even at low PSA levels (for example, below 0.2 ng/mL).
However, the decision always depends on the individual disease course and the specific clinical question.
How High Is the Radiation Exposure from a PSMA PET/CT?
Radiation exposure is comparable to that of other diagnostic nuclear medicine and radiological examinations. When there is a clear medical indication, the benefit significantly outweighs the low theoretical risk. An individualized consultation is provided prior to the examination.
Do I Need to Fast Before a PSMA PET/CT Scan?
In most cases, no special fasting is required. You will receive individual preparation instructions in advance.
When Will I Receive the Results of My PSMA PET/CT?
The evaluation is performed promptly by our experienced nuclear medicine specialists. The report is prepared in a timely manner and discussed with you and/or your treating physician.
Will PSMA PET/CT Be Covered by Health Insurance?
Coverage depends on the medical indication and your specific health insurance provider. Individual clarification is provided as part of the appointment scheduling process.
We take time for what matters - your care
If you have questions or would like to schedule an appointment, we are here for you.
In a personal consultation, we discuss your concerns in a calm setting and outline the next steps together.
Our team will get back to you promptly and support you competently and reliably - from the first contact through to your therapy appointment.

We're here for you
Do you have questions or would you like to schedule an appointment?
We take the time to understand your concerns and will get back to you promptly.
Contact Details
Do you have questions about PSMA therapy? Contact our team for further information or to schedule an appointment.
Phone
Adress
Heiligenstädter Str. 55/65
1190 Vienna - Austria



