Prostate Cancer – Symptoms, Diagnosis, Staging, and Treatment
Prostate cancer is the most common cancer in men worldwide and develops from cells of the prostate, a small gland located below the urinary bladder. In its early stages, the disease often causes no or only non-specific symptoms, which is why it is frequently detected during PSA screening or routine urological examinations.
Accurate diagnosis is essential to distinguish between slow-growing tumors and those requiring treatment—and to enable the targeted use of modern therapeutic approaches in more advanced stages.
In this article, we explain the key concepts in a clear and accessible way—and show when PSMA PET/CT, as an advanced form of molecular imaging, can be a valuable addition.

What is prostate cancer?
The prostate is a walnut-sized gland located below the bladder that surrounds the beginning of the urethra. It produces part of the seminal fluid and is primarily regulated by the hormone testosterone. Changes in the glandular cells can lead to uncontrolled cell growth—resulting in prostate cancer.
Not all prostate cancers behave the same. Some tumors grow very slowly and may remain confined to the prostate for years, while others are more aggressive and can spread early to surrounding tissues or distant organs. These differences make careful diagnosis and individualized risk assessment essential.
Known risk factors include:
- increasing age
- family history (e.g., prostate cancer in a father or brother)
- certain genetic alterations (e.g., BRCA mutations)
- hormonal influences
- smoking
Important to know: The presence of a risk factor does not automatically mean that cancer will develop—it only increases the likelihood.
Because early-stage prostate cancer often causes no clear symptoms, structured evaluation through PSA testing, clinical examination, and—when necessary—advanced imaging plays a key role. Modern diagnostic methods help to accurately assess the extent of disease and guide the most appropriate treatment strategy.
Incidence and Epidemiological Significance of Prostate Cancer
Prostate cancer is the most common cancer in men worldwide. According to current estimates by the International Agency for Research on Cancer (IARC), approximately 1.47 million new cases are diagnosed each year (GLOBOCAN 2022).
In Austria, prostate cancer is the most common malignant tumor in men. Approximately 6,000 to 6,500 new cases are diagnosed annually. Around 1,200 to 1,300 men die each year as a result of the disease. In total, an estimated 70,000 to 75,000 men in Austria are currently living with a diagnosis of prostate cancer (Statistics Austria, Austrian Cancer Registry, most recently published prevalence data). This means that prostate cancer accounts for approximately one quarter of all newly diagnosed cancers in men.
Symptoms of Prostate Cancer – Early Signs and Warning Signals
In its early stages, prostate cancer often causes no clear or specific symptoms. Many tumors are therefore detected incidentally during routine screening or due to an elevated PSA level. This lack of early symptoms makes structured urological evaluation particularly important.
Early, often non-specific symptoms
When symptoms do occur, they usually affect urination. These may include:
- a weak or interrupted urine stream
- increased urinary frequency, especially at night
- difficulty initiating urination
- a feeling of incomplete bladder emptying
However, these symptoms are not specific to cancer and are also commonly seen in benign prostate enlargement.
Symptoms in advanced stages
In more advanced stages or in the presence of metastases, additional symptoms may occur, such as:
- blood in the urine or semen
- pain in the pelvis, lower back (lumbar spine), or bones
- unexplained fatigue or weight loss
Bone pain may occur particularly when cancer cells have spread to the skeleton—a common site of metastasis in advanced prostate cancer.
It is important to note that these symptoms may also be caused by other conditions unrelated to prostate cancer. Nevertheless, men experiencing persistent or unusual symptoms should seek medical evaluation to determine the cause. Early detection of prostate cancer is typically achieved through regular screening, primarily by measuring prostate-specific antigen (PSA) levels and performing a digital rectal examination.
When should a medical evaluation be performed?
A timely urological assessment is recommended in the following cases:
- newly occurring or worsening symptoms during urination
- a persistently elevated or rising PSA level
- a family history of prostate cancer
Early diagnostic evaluation makes it possible to distinguish between slow-growing tumors and more aggressive forms that require treatment. Modern imaging—such as PSMA PET/CT—can provide additional clarity, particularly when metastases are suspected or when PSA levels rise again after therapy.
Diagnosis of Prostate Cancer
If prostate cancer is suspected, the diagnostic process is carried out in several sequential steps. The goal is to establish a reliable diagnosis, determine the extent of the disease, and enable a well-founded treatment decision.
The PSA Level
Prostate-specific antigen (PSA) is a protein produced by prostate cells and measurable in the blood. An elevated or rising PSA level may indicate prostate cancer—but can also be caused by benign conditions or inflammation. Therefore, it is not only the single value that matters, but above all:
- its development over time
- the rate of increase (PSA doubling time)
- the overall clinical context
An elevated PSA level alone does not constitute a cancer diagnosis, but rather an indication for further investigation.
Clinical Examination and MRI of the Prostate
The digital rectal examination (DRE) allows the urologist to palpate the prostate for indurations or nodules. In addition, multiparametric MRI (mpMRI) of the prostate is now frequently used. This imaging technique can make suspicious areas visible and helps to plan a targeted biopsy.
Biopsy
Only tissue sampling (biopsy) provides histological confirmation of prostate carcinoma. The obtained tissue is examined under the microscope and evaluated according to the Gleason score or ISUP grading system. This classification provides information on how biologically aggressive the tumor is.
Staging
Once the diagnosis has been confirmed, it is assessed whether the tumor is confined to the prostate or has already spread. Depending on the clinical situation, different diagnostic methods are used, for example:
- MRI or CT to assess local tumor extent
- bone scintigraphy if bone metastases are suspected
- advanced molecular imaging such as PSMA PET/CT, particularly in advanced stages or in the case of a rising PSA level
Especially when metastases are suspected or findings are inconclusive, PSMA PET/CT can provide additional, more precise information and thus significantly influence treatment planning.
Stages and Risk Groups
After a confirmed diagnosis, the key question arises: How advanced is the disease, and how aggressive is the tumor? This assessment has a decisive influence on the choice of therapy.
TNM System – Systematically Assessing Tumor Spread
The TNM system describes the stage of the disease:
- T (Tumor): How large is the tumor, and is it confined to the prostate?
- N (Nodes): Are lymph nodes affected?
- M (Metastases): Are there deposits in distant organs, such as the bones or liver?
A localized tumor (e.g., T1–T2, N0, M0) differs significantly in terms of treatment from prostate cancer that has already metastasized.
Gleason Score and ISUP Grading
The Gleason score is based on the microscopic evaluation of tumor tissue. It indicates how much the cancer cells differ from normal prostate tissue.
- Lower scores are associated with slowly growing tumors.
- Higher scores indicate more aggressive tumor biology.
Today, the ISUP grading system (Grade Groups 1–5) is also frequently used to classify aggressiveness more precisely.
Risk Groups
For treatment planning, PSA level, tumor stage (TNM), and Gleason/ISUP grade are combined. This results in simplified risk categories:
- Low risk: often suitable for active surveillance
- Intermediate risk: individualized treatment decision
- High risk: usually requires active, more intensive therapy
In advanced or metastatic prostate cancer, precise assessment of tumor burden and distribution becomes increasingly important. PSMA PET/CT can help to accurately detect even small metastases and to guide treatment planning in a targeted manner.
Accurate staging is essential to avoid both overtreatment and delays in necessary therapy.
Metastases in Prostate Cancer
In advanced stages, prostate cancer can spread beyond the prostate. Tumor cells may travel via the lymphatic system or blood vessels to other parts of the body, where they form so-called metastases. Understanding these patterns of spread is crucial for selecting the appropriate therapy.
Common Sites of Metastases
In prostate cancer, metastases most commonly occur in:
- bones (spine, pelvis, ribs)
- lymph nodes in the pelvic or abdominal region
- less frequently in the liver or lungs
Bone metastases are the most common and can lead to load-dependent or persistent pain.
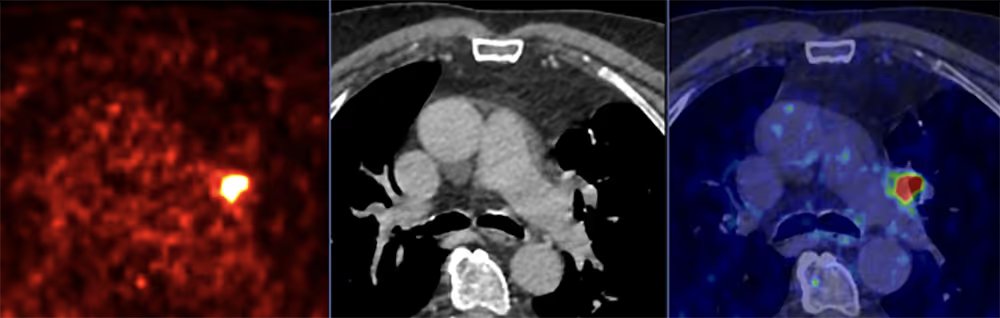
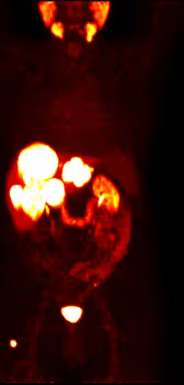
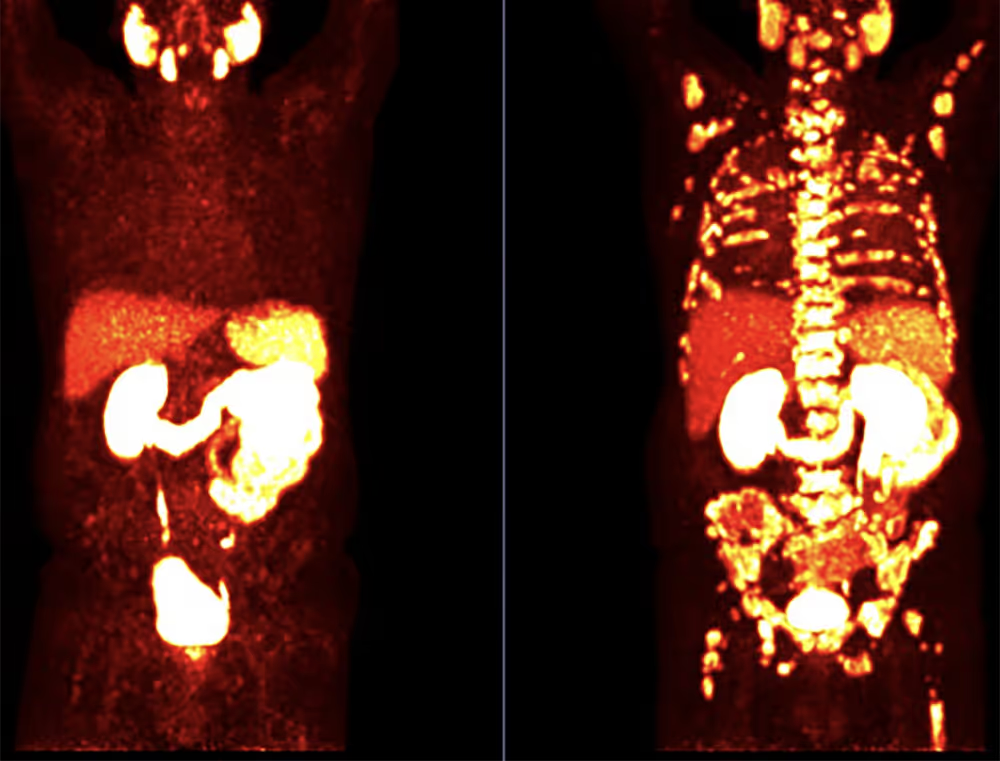
PSMA PET/CT LEFT: Near-complete remission after 6 cycles of ^177Lu-PSMA therapy (PSA tumor marker decreased to 3.0 ng/mL).
Possible Symptoms of Metastases
Not every metastasis causes symptoms immediately. If symptoms occur, they may present as:
- persistent or increasing bone pain
- restricted mobility
- general weakness or fatigue
- anemia in cases of extensive bone involvement
In the presence of neurological symptoms such as numbness or signs of paralysis, prompt medical evaluation is required.
How Metastases Are Diagnosed
Various imaging techniques are used to assess the extent of disease spread:
- CT or MRI to visualize organs and lymph nodes
- bone scintigraphy if skeletal involvement is suspected
- PSMA PET/CT as a modern molecular imaging modality to detect even small or difficult-to-visualize metastases
Particularly in cases of rising PSA levels after prior therapy or when advanced disease is suspected, PSMA PET/CT can provide a more precise assessment of tumor distribution.
Accurate detection of metastases is essential in determining whether local, systemic, or targeted molecular therapy—such as PSMA radioligand therapy—is appropriate.
Treatment Options for Prostate Cancer
The treatment of prostate cancer depends on several factors: tumor stage, biological aggressiveness (Gleason/ISUP), PSA dynamics, the presence of metastases, and the patient’s overall health status. Not every diagnosis automatically requires immediate intensive treatment—the therapy is planned individually.
Active Surveillance
In tumors with low risk and favorable biological characteristics, close monitoring may be appropriate. This includes regular PSA testing, MRI examinations, and, if necessary, repeat biopsies. The goal is to avoid overtreatment and to initiate active therapy only if there are signs of disease progression.
Surgery – Radical Prostatectomy
In localized prostate cancer, complete removal of the prostate can be a curative option. The procedure is performed either as open surgery or robot-assisted. Possible risks include, among others, urinary continence and erectile function, which is why careful preoperative counseling is essential.
Radiation Therapy
External beam radiation therapy or brachytherapy (placement of radioactive sources directly into the prostate) are established alternatives to surgery—particularly in localized or locally advanced tumors.
Hormone Therapy and Modern Androgen Receptor–Targeted Therapies
Since prostate cancer is usually hormone-dependent, androgen deprivation therapy (ADT) can slow tumor growth. In advanced stages, modern medications are additionally used that specifically target androgen metabolism.
Chemotherapy
In metastatic or castration-resistant prostate cancer, chemotherapy (e.g., with Docetaxel or Cabazitaxel) may be part of the treatment strategy.
PSMA Radioligand Therapy – Targeted Molecular Treatment
In advanced or metastatic prostate cancer, PSMA radioligand therapy can represent an additional treatment option. In this approach, a radioactively labeled molecule binds specifically to PSMA-expressing tumor cells and destroys them from within. A prerequisite is usually sufficient PSMA expression, which is assessed beforehand using PSMA PET/CT.
The choice of the most appropriate therapy in an individual case should always be made in an interdisciplinary setting and based on a comprehensive evaluation of all findings.
Prognosis and Disease Course
The prognosis in prostate cancer depends strongly on the stage at the time of diagnosis and on the biological characteristics of the tumor. Many tumors confined to the prostate grow slowly and can be very well controlled or treated if detected early. In advanced stages, the goal is often to slow disease progression, alleviate symptoms, and preserve quality of life for as long as possible.
Key Factors Influencing Prognosis
Several factors play a role:
- Tumor stage (TNM): Is the cancer confined to the prostate, or has it already metastasized?
- Gleason score / ISUP grade: How aggressive do the tumor cells appear under microscopic examination?
- PSA kinetics: How rapidly is the PSA level rising?
- Tumor burden and pattern of metastasis: Number and location of metastases
- General health status and comorbidities
These factors are not assessed in isolation but are evaluated in an overall clinical context. Especially in metastatic prostate cancer, precise imaging - such as PSMA PET/CT - can help to more accurately assess the true extent of disease and to make more targeted treatment decisions.
Why Follow-Up Monitoring is important
Even after therapy, regular follow-up examinations remain essential. These include:
- PSA monitoring at defined intervals
- Imaging studies if there is suspicion of disease progression
- Clinical assessment of symptoms
A renewed rise in PSA does not automatically require an immediate change in therapy, but it should be carefully evaluated. Modern diagnostic methods now make it possible to detect recurrence at an early stage and to treat it in a targeted manner.
A realistic and transparent assessment of prognosis is an integral part of responsible medical counseling. Our goal is to work together to choose a treatment strategy that is medically appropriate while also taking your individual situation into account.
Living with Prostate Cancer – Daily Life, Quality of Life and Support
A diagnosis of prostate cancer affects not only the body, but often also emotional well-being, relationships, and everyday life. Alongside medical decisions, quality of life and individual needs therefore play a central role.
Sexual Function
Depending on the type of treatment, changes in erectile function or ejaculation may occur. Hormonal therapies can also affect libido and overall sexual function. These effects are well understood in medicine and should be addressed openly and without hesitation. A range of supportive measures and therapeutic options is available to help maintain quality of life.
Urinary Continence and Physical Changes
After surgery or radiation therapy, temporary or permanent impairments in bladder control may occur. Pelvic floor training and specialized physiotherapy programs can be beneficial in improving continence. Fatigue—persistent physical and mental exhaustion—is also a possible side effect, particularly during systemic treatments.
Emotional Well-Being and Psychological Support
Uncertainty about the course of the disease, treatment decisions, or rising PSA levels can be emotionally challenging. Open communication with your medical team, psycho-oncological support, and connecting with other patients or support groups can help you cope more effectively with the situation.
Living with Advanced Prostate Cancer
In metastatic prostate cancer, symptom relief becomes a central focus alongside tumor control. Effective pain management, targeted medical treatment, and an individually tailored therapy plan help preserve mobility and quality of life for as long as possible.
Structured care, regular follow-up assessments, and transparent communication are essential to jointly establish a safe and clearly understandable treatment pathway.
Prostate Cancer Care at Theranosticum Vienna
Not every case of prostate cancer requires specialized nuclear medicine diagnostics or therapy. However, in certain situations, more advanced evaluation can be crucial to gain clarity and to plan the next steps in a targeted and well-informed manner.
A consultation at our specialized center may be particularly beneficial in the following situations:
- Rising PSA levels after prior treatment (suspicion of recurrence)
- Unclear metastatic status when conventional imaging does not provide definitive results
- Advanced or metastatic prostate cancer, where modern, targeted treatment options should be carefully evaluated
PSMA PET/CT imaging can help to accurately visualize the true extent and distribution of disease, thereby enabling well-informed treatment decisions. Based on these findings—and if medically appropriate—PSMA radioligand therapy may also be considered.
At Theranosticum Vienna, each case is evaluated in a structured and interdisciplinary setting. Our goal is to assess all available findings within their full clinical context and to provide a transparent recommendation—realistic, clearly understandable, and tailored to your individual situation.
Frequently Asked Questions About Prostate Cancer
In the context of a prostate cancer diagnosis, many similar questions often arise. Clear and understandable information can help reduce uncertainty and support well-informed decision-making.
How Fast Does Prostate Cancer Grow?
Tumor growth can vary considerably. Some tumors develop slowly over many years and remain confined to the prostate, while others show more aggressive behavior. Key factors influencing growth include the Gleason score/ISUP grade, tumor stage, and PSA dynamics over time.
What Does a Rising PSA Level Mean?
A single elevated PSA level is not, by itself, proof of cancer. What matters most is how PSA levels change over time. After treatment, a renewed rise in PSA may indicate a recurrence and should be further evaluated—potentially using advanced imaging such as PSMA PET/CT.
Can Prostate Cancer Be Cured?
In cases where prostate cancer is confined to the prostate, there is often a high likelihood of cure through surgery or radiation therapy. In more advanced stages, the focus typically shifts toward long-term disease control and maintaining quality of life.
When Is PSMA PET/CT Useful?
PSMA PET/CT can be particularly helpful in cases of unclear metastatic status, advanced disease, or rising PSA levels following prior treatment. It provides a highly accurate assessment of disease distribution and can significantly influence treatment planning.
Who Is a Candidate for PSMA Therapy?
PSMA radioligand therapy is typically considered in patients with advanced or metastatic prostate cancer. A key requirement is sufficient PSMA expression, which is confirmed through prior imaging. Eligibility should always be assessed on an individual basis within an interdisciplinary setting.
If you are unsure how to interpret your findings, a professional medical assessment by our clinical team can provide clarity and guidance.
Ihre nächsten Schritte
Following a diagnosis of prostate cancer, many decisions need to be made. The most appropriate treatment depends not only on the stage of the disease, but also on the biological characteristics of the tumor, previous treatments, PSA dynamics, and your overall health. Looking at individual findings in isolation is often not sufficient—what matters is the overall clinical picture.
A professional medical assessment can help to:
- Interpret your current findings in a medically meaningful context
- Realistically assess the actual stage of the disease
- Weigh appropriate diagnostic and therapeutic options
- Clarify open questions in a clear and understandable way
At Theranosticum Vienna, this evaluation is based on all available information - transparent, evidence-based, and tailored to your individual situation.
We focus on the person as a whole, not just the disease.
If prior reports, PSA trends, or imaging results are already available, they can be reviewed in detail and discussed together.
We take time for what matters - your care
If you have questions or would like to schedule an appointment, we are here for you.
In a personal consultation, we discuss your concerns in a calm setting and outline the next steps together.
Our team will get back to you promptly and support you competently and reliably - from the first contact through to your therapy appointment.

We're here for you
Do you have questions or would you like to schedule an appointment?
We take the time to understand your concerns and will get back to you promptly.
Contact Details
Do you have questions about PSMA therapy? Contact our team for further information or to schedule an appointment.
Phone
Adress
Heiligenstädter Str. 55/65
1190 Vienna - Austria



